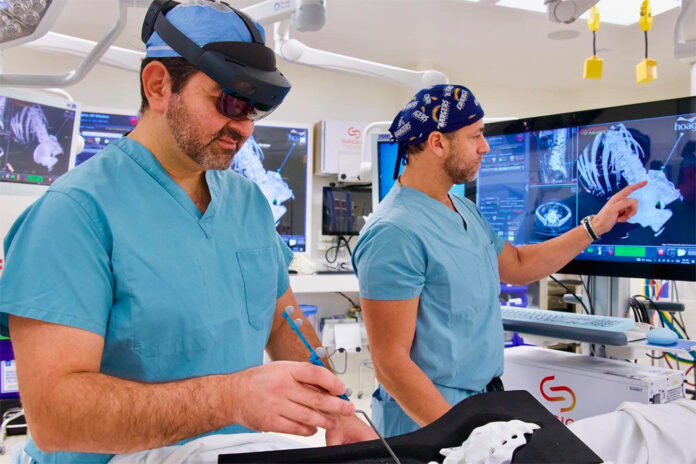
A hologram helped a pair of surgeons in Newport Beach conduct what they say is their first spinal surgery using their own developed augmented reality (AR).
Dr. Burak Ozgur, director of Hoag Memorial Hospital Presbyterian’s Spine Center at the Pickup Family Neurosciences Institute, and Dr. Adam Kanter, associate executive medical director of the institute, performed the first spinal fusion surgery utilizing augmented reality technology called SyncAR.
“The beauty of this is now I can see the patient’s spine before we’ve made any incision,” Ozgur said. “I can plan out where my cuts are going to be, the size of screws, the depth, the length.
FDA Clearance
Hoag’s neurosurgeons worked with a Cleveland company called Surgical Theater to develop the visualization platform. Its cost to develop hasn’t been disclosed.
The doctors studied and published the benefits of SyncAR technology in the lab, demonstrating an improved accuracy of more than 99% for screw placement in the spine, helping it receive FDA clearance in September.
“Integrating augmented reality into the operating room has the potential to improve surgical precision and patient outcomes at hospitals around the world,” Ozgur said.
“SyncAR for Spine is allowing not only enhanced navigation in the operating room, it is enabling more enlightened and informed pre-operative conversations with our patients.”
No Room for Errors
In typical spine surgeries, doctors use CT or MRI scans that are two-dimensional, Ozgur said. Doctors would have to make long incisions to open the back to see where the problems existed.
“Traditional spine surgery scares people because most incisions are going to be really big and you’re going to be suffering in the hospital for days, weeks, and then months of recovery,” Ozgur said.
Spinal surgery isn’t for the faint of heart.
“If you’re a little off, you might hit the spinal cord, which paralyzes the patient,” he said. “If you go this way, you might hit other vital organs or blood vessels.
“Any technology where we can track the equipment is going to make the outcome better.”
Prep Assistance
The hologram software helps the doctors to both prepare for the surgery, and then during the surgery itself.
The program uses CT and MRI images of the patient that are then cut into various small segments and recreated in a 3D view to produce a hologram that is a life-like reconstruction of the spine.
During a demonstration given to the Business Journal, the hologram was a replica of the person’s actual spine without the skin blocking the view. The doctors could spin the hologram as though it was in a “Star Wars” movie.
“I don’t want to use the word ‘X-ray vision,’” Kanter said. “It’s the ability to accurately see where you’re going with great precision.”
The hologram allows the doctors to rehearse what they will do during surgery.
“Without opening up the patient, we can now see what their spine looks like,” Ozgur added.
“When you add augmented virtual reality, we can maybe make incisions even smaller and do even more complex things that we couldn’t do before because now we can visualize it.”
Surgery Sight
Ozgur and Kanter gave a demonstration of how augmented reality would work during surgery, using a model of a body and the instruments that guide incisions.
During the surgery, the surgeon wears a hat shaped like a visor that covers the top half of the doctor’s vision. By glancing down, the doctor can see the patient and where the incisions are in the body. By glancing up, the doctor can see the hologram and other key data points like blood pressure.
“In surgery, a lot of times we are operating but then we’ve got to swing our head around and look at the screen and we may want to look at the blood pressure and we may want to look at so many different things,” Ozgur said.
“Anytime we can have technology help us make it easier, safer and faster, we’re all for it.”
Cranial Work
Ozgur and Kanter said they believe this technology can be used on any body part.
The pair adapted AR technology from cranial surgery being done by Dr. Robert Louis, Hoag’s chief of neurosurgery and the Empower360 Endowed Chair in Skull Base and Minimally Invasive Neurosurgery, and Dr. Daniel Yanni, vice chair of the division of neurosurgery.
“Much of the discussion of surgical innovation centers around the next hardware iteration,” Yanni said. “Few people think, ‘How do we change surgical execution?’ It takes a hospital as forward-thinking as Hoag to advance the way surgery is conducted.”
Kanter and Ozgur typically perform about 10 spinal surgeries a week. This new technology won’t be for every surgery, they said.
“It’s like a cellphone, which was like a brick when it was introduced. Every year, it got better,” Ozgur said.
“For spines, it’s just the beginning. It’s going to get better than it already is. We’re excited about it.”
The pair said the first patient to receive spinal surgery with the assistance of a hologram is recovering well.
Editor’s Note: This article has been corrected to note that Hoag Hospital wasn’t the first worldwide to conduct augmented reality spinal surgery. Instead, it was the first time that it used its own software for augmented reality spinal surgery. Augmedics, an Illinois-based company, contacted the Business Journal to say its software was used to conduct the world’s first spinal surgery at Johns Hopkins Hospital in 2020.