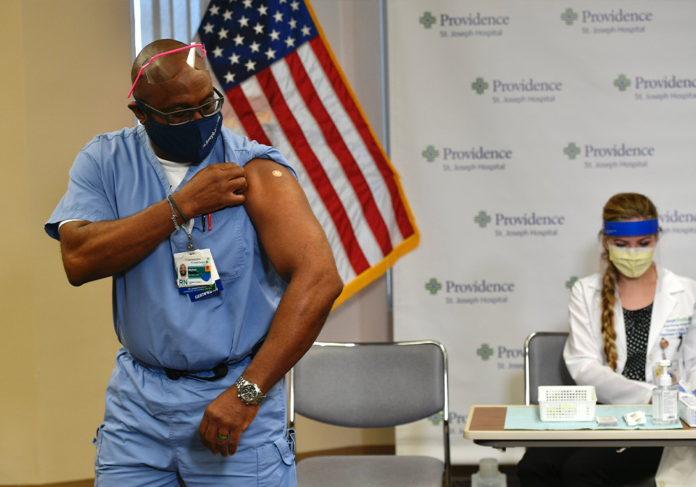
Orange County continued to see a surge in COVID patients as the first batch of vaccines arrived last week.
“Soon, we will be protecting all of our caregivers in our community and eradicating this horrific pandemic,” Erik Wexler, chief executive of Providence Southern California, said at a press conference where the first healthcare workers in OC were given the Pfizer vaccine last Wednesday.
It’s a much-needed victory for OC’s largest hospitals, which have been put under an enormous amount of pressure adjusted; intensive care unit capacity fell to 0% as of late last week.
Of the county’s 628 adult ICU beds, about 51% (or 319 patients) were occupied by COVID patients and 40% (or 246 patients) were filled by individuals with other critical conditions, as of last Tuesday.
ICUs are typically comfortable operating at 50% capacity, multiple hospital officials confirmed.
Below is a closer look at how OC’s healthcare community is responding to the continued COVID surge with field hospitals, non-acute care facilities and caregiver resources.
Field Hospitals
OC’s largest hospitals have put into action plans to grow ICU capacity between 20% to 50%.
“As with hospitals everywhere, Kaiser Permanente’s hospital ICUs are heavily impacted by the current surge in COVID-19 cases. Capacity fluctuates daily–even hourly—and we have plans and space identified to expand bed capacity if needed,” said Mark Costa, senior vice president and area manager for Kaiser Permanente Orange County.
In addition, last week several hospitals requested additional support from the county.
Providence’s St. Jude Medical Center of Fullerton has been particularly hard hit and reported its ICU was full at 105% capacity. It’s receiving triage support from the county, as well as a 25-bed mobile field hospital—a tent with hard flooring and temperature-controlled units.
UCI Medical Center in Orange and Fountain Valley Regional Hospital are also set to receive 50-bed mobile units. Filings indicate Hoag Memorial Hospital Presbyterian and Providence’s St. Joseph Hospital are prepared to add field units as well.
The county, which has the ability to deploy eight mobile hospitals that support at a minimum 200 beds, also last week suspended ambulance diversion. This means hospitals cannot send ambulances away.
The order came about after nearly all hospitals were diverting ambulances, the county said.
Non-Acute Facilities
The ICU story is a similar one for overall hospital capacity.
Hospitalized patients with COVID, including ICU patients, was about 1,310 per day on average last week in OC.
Indoor facilities have been repurposed where appropriate.
Hoag Hospital for instance is using its gift shops, which have been closed due to visitor restrictions, for routing COVID screenings for staff members.
“This is a time for being flexible and adapting to change, and our health care facilities are no different,” said Robert Braithwaite, chief executive of Hoag.
CHOC Children’s started taking young adults—defined as patients under the age of 29 years old—into its hospital about a week ago. Its main hospital in Orange is within minutes of St. Joseph Hospital and UCI Medical Center.
Fairview Alternative Care Site in Costa Mesa also opened for non-acute COVID patients.
The county-run site has 125 beds for patients that have passed the critical stage in hospitalization and no longer need equipment and treatment that demands an ICU bed, the county said.
A 25-bed unit within Fairview is expected to launch for patients with dementia as soon as Dec. 28.
It will be operated by Alzheimer’s Association of OC to provide safe and effective care to patients with memory loss, who are often asymptomatic and don’t need intensive care resources, said Chief Executive Jim McAleer.
Caregiver Concerns
Hospitalization rates have put an unprecedented pressure on healthcare workers.
It’s not uncommon to hear caregivers going through a routine, putting all of their clothing and belongings into a bucket in their garage before entering their house, or even sleeping in their car, because they don’t want to bring the virus home to their family members, said Jeremy Zoch, chief executive of St. Joseph Hospital.
Nurses with non-critical care roles have volunteered to help, even serving as runners to communicate between patients and their families, he said.
Several hospitals have submitted waivers to operate at reduced nurse-to-patient ratios. California is one of the few states that mandates a nurse-to-patient ratio of 1:2 in ICUs and 1:5 in surgical care units. These waivers allow hospitals to operate at a nurse-to-patient ratio of 1:3 in ICUs and 1:7 in surgical care units.
Others have operations centers in place to move personnel between units and even hospitals as needed to ensure caregivers get breaks and time in between shifts.
Hospitals are also providing additional resources to liven caregivers’ spirits. UCI Health for example is providing virtual yoga and meditation, free daycare, household supplies (during the last stay-at-home order) and meals.