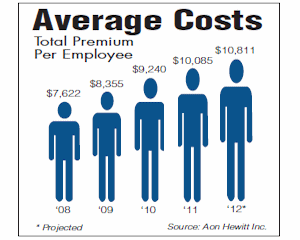
The increase in the amount employers in Orange County will pay toward insurance premiums for workers is expected to average 7.2%—about $800 apiece—next year.
That will put the average here at $10,811 per employee, according to a recent report from Aon Hewitt Inc., a Chicago-based human resources consulting company.
The bump here is expected to be slightly higher than the national average, which is expected to rise 7%, to $10,475 per worker.
The expected increase would be the smallest since 2008, when businesses averaged a hike of 7%.
It also would be down from this year’s increase, which came to an average of 9.1% for businesses here, according to Aon Hewitt.
The smaller increase expected for 2012 appears to reflect ramifications of the healthcare reform that became federal law in 2010 and has affected the market in phases since. One key factor: lower use of employer-based insurance programs.
“The impacts of healthcare reform in 2011 were more significant than in 2012, and the other is that we have seen trend decrease slightly across the board, primarily due to utilization decreases,” said Lee Reichenbach, the Newport Beach-based leader of Aon Hewitt’s Southern California local practice.
Another factor that affected premiums in 2011 included a new requirement that dependent children up to age 26 could be carried on their parents’ plan. The additional costs of carrying older children were priced into many plans.
Pushing Prices
Reichenbach said increasing healthcare service costs, more use of pricey specialty drugs, and the demographic trend of an aging work force all help push costs up.
Rick Grant, chief executive of MobileNet Services Inc., an Irvine radio frequency engineering and testing company that serves wireless providers, expects his company’s healthcare insurance premiums to go up 10% on average.
MobileNet just finished renewing its healthcare plan last month.
Grant said he thinks the increase in costs for insuring the company’s 180 workers has little do with usage rates or demographic trends.
“I have a pretty young work force,” he said. “I think (the premium hike’s) just typical of the (healthcare) industry.”
MobileNet offers a variety of health plans from Anthem Blue Cross. It has Principal Dental for its dental care.
It was originally faced with a 12% increase in its health maintenance organization plan. It got a lower rate with a move to Anthem Blue Cross’ select-network plan, which has a tighter selection of doctors and hospitals.
MobileNet is splitting the increase with workers, Grant said.
Decliners?
Some employers believe their costs will go down in 2012.
MS International Inc. Vice President Raj Shah said the company is “extremely early” in its bid process, “but I expect (our) healthcare costs to go down because we have implemented a very significant wellness program.”
The Orange-based wholesaler of natural stone for construction, which has 225 local workers, offers an HMO plan through Kaiser Permanente and a preferred-provider plan from Blue Shield of California, Shah said. It funds its own vision insurance claims, and offers dental insurance coverage through Cigna.
Shah said his company pays 80% of its workers’ health plans, and does not plan to change its contribution.
Kaiser, an Oakland-based health plan that operates the county’s largest HMO with 392,000 non-Medicare members, expects its clients will pay between 6% and 8% more for insurance in 2012, depending on the size of groups, said Juan Lopez, the plan’s area director of sales and marketing.
Kaiser does not anticipate any healthcare reform-related pricing in its plans until August 2012, when the law requires insurers to provide “well woman” coverage at zero cost to members, Lopez said.
The insurer has priced healthcare reform into its coverage in recent years, including the dependent increase and “zero preventative (healthcare) charges,” he said.
Kaiser clients are handling the rate increases in various ways, according to Lopez.
“Some clients, depending on the type of business, are absorbing the majority of the increase, but they’re definitely cost-sharing with their employees,” Lopez said.
Aon Hewitt’s data bears that out.
The company’s figures show that Orange County workers, on average, will pay $2,448 for their portion of health insurance coverage in 2012, up about 11% from this year’s $2,205.
“Employers in Orange County have been a little bit more aggressive in passing on cost increases,” Reichenbach said.
Smaller numbers of union workers here compared to other parts of the country is one reason employers here have been able to pass along more costs, she said.
The outlook for another insurer with operations here falls in line with Aon Hewitt’s report.
“For the most part, we’re seeing average increases in the single digits,” said Cheryl Randolph, a spokeswoman for UnitedHealth Group Inc., a Minneapolis-based insurer with a large operation in Cypress and an estimated 221,000 HMO and PPO members in Orange County.
UnitedHealth clients’ premium increases will vary by the particular market, type of plan and employer size, Randolph said.
At Newport Beach-based Nixon Benefits, owner Karen Nixon said next year’s rate increases for her clients are hovering around 10% for groups of 100 to 500 people and around 5% to 6% for businesses with 500 or more workers.
“It’s still going up because health reform just addressed insurance and not the cost of care,” Nixon said. She cited a recent Congressional Budget Office study showing that the cost of healthcare will go up 26% over the next four years.
“Insurance will have to start reflecting that,” Nixon said.
Moderate View
Some industry professionals expect more moderate increases next year.
“In some cases, the rates have decreased,” said Kelly Moore, president of Moore Benefits Inc. in Irvine, which specializes in clients with 200 or fewer employees.
“I haven’t seen that since the ’90s, when HMOs became popular,” Moore said.
The slower rate of increase expected next year has “a lot to do” with requirements that compel health insurers to spend at least 80% of every premium dollar they collect on patient care, she said. The requirement goes up to 85% for large groups.
Moore also said it appears that some workers are using their benefits less.
She noted that most smaller employers are sticking with commercial carriers, with some self-funding plans that are cheaper but have very high deductibles to offer alongside standard packages.